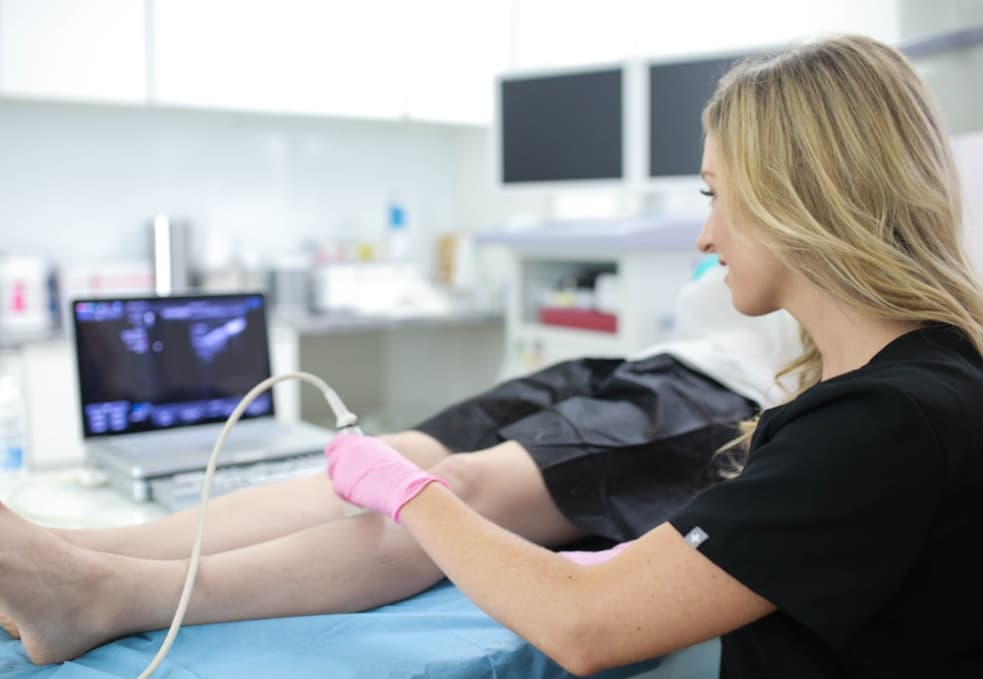
Are you tired of dealing with the discomfort and unsightly appearance of varicose veins? Long Island Vein Treatment is here to help. As a group of medical centers led by board-certified vein doctors, we specialize in minimally invasive treatments for varicose and spider veins, such as sclerotherapy, endovenous laser ablation, radiofrequency ablation, and phlebectomy. We understand that treating varicose veins is only part of the equation – preventing them from coming back is equally important. In this guide, we will walk you through effective strategies to prevent varicose veins from making a return appearance.
First, Can You “Prevent” Varicose Veins?
While there are certainly strategies and lifestyle changes that can significantly reduce the risk of developing varicose veins, it’s essential to understand that there are no foolproof methods to guarantee their prevention or ensure they won’t reappear once treated. Varicose veins, often caused by weakened vein walls and malfunctioning valves, can be influenced by a combination of genetic, hormonal, and lifestyle factors. While you can control some of the risk factors for varicose veins, such as your lifestyle, others like genetics are out of your control.
However, this doesn’t mean you should be discouraged. By adopting proactive measures and making healthy choices, you can dramatically minimize your risk and improve your overall vein health. It’s essential to remember that even if varicose veins develop or return despite your efforts, there are effective medical interventions available to manage and treat them.
Why Varicose Veins Often Recur After Treatment
The Appearance of New Varicose Veins
Even after successfully treating varicose veins, it’s not uncommon for new ones to appear over time. These fresh varicose veins can develop independently in different areas of the legs. Several factors contribute to their formation, including genetics, age, hormonal changes, and lifestyle choices. While the treatment of existing varicose veins can provide relief, staying vigilant and adopting preventive measures remains crucial to managing the risk of new varicose veins emerging in the future.
Not Treating Venous Insufficiency During the Primary Treatment
One significant reason for varicose veins returning after treatment is the failure to adequately address underlying venous insufficiency during the initial intervention. When the root cause, such as chronic venous insufficiency (CVI), remains untreated, it can lead to the development of new varicose veins or the resurgence of previously treated ones. As such, you must contact vein doctors who perform thorough diagnostic tests like duplex ultrasound to identify and treat underlying vein disease before treating superficial varicose veins.
Other Risk Factors for Varicose Veins:
- Family History: Genetics can play a substantial role in determining your susceptibility to varicose veins. This genetic link suggests that certain structural aspects of your veins may be inherited, making them more prone to weakening and valve dysfunction.
- Pregnancy: Hormonal fluctuations can exert an influence on vein health. Pregnancy triggers hormonal changes that affect the elasticity of blood vessel walls and the tone of vein valves. The combination of increased blood volume and pressure on the veins during pregnancy can lead to the development of varicose veins.
- Inactivity: A sedentary lifestyle can contribute to varicose veins by impeding proper blood circulation. When you spend long hours sitting or lying down, your calf muscles don’t contract as frequently, making it harder for blood to flow upward against gravity.
- Tight Clothing: Wearing tight clothing, particularly garments that compress the waist and legs, can hinder blood flow. This constriction can increase the risk of varicose veins, as it puts additional pressure on the veins, making it more challenging for blood to circulate freely.
- Smoking: Smoking has a detrimental effect on blood vessels and overall cardiovascular health. It damages the inner lining of blood vessels, making them less flexible and more prone to dysfunction. This, in turn, can exacerbate venous issues and raise the risk of developing varicose veins. Quitting smoking can significantly improve vein health.
- Injury or Trauma: Previous injuries or trauma to the legs can disrupt the normal functioning of veins. Scar tissue or damage to the veins themselves can impede blood flow and increase the likelihood of developing varicose veins.
Effective Ways to Reduce the Risk
Maintain a Healthy Weight
Maintaining an optimal body weight is a crucial factor in preventing varicose veins. Excess weight places undue pressure on your veins, especially those in your legs, as they have to work harder to return blood to your heart. This increased pressure can weaken vein walls and valves, making them more susceptible to malfunction. Adopting a balanced diet that promotes weight management and engaging in regular physical activity can help you sustain a healthy weight, reducing the risk of varicose veins.
Exercise Regularly
Regular physical activity plays a pivotal role in preventing varicose veins. Exercise not only enhances overall cardiovascular health but also strengthens the muscles in your legs. Strong leg muscles assist in pumping blood more effectively back to your heart, reducing the strain on your veins. Incorporate at least 30 minutes of moderate exercise, which can include walking, swimming, cycling, or specific leg exercises.
Elevate Your Legs
Elevating your legs can alleviate the pressure on your veins and improve blood circulation. Elevating your legs, especially after a long day of standing or sitting, encourages blood to flow more freely from your lower extremities back toward your heart. To do this, lie down and prop your legs up on a pillow or cushion, ensuring they are elevated above the level of your heart. This can significantly reduce the risk of varicose veins.
Avoid Prolonged Sitting or Standing
Jobs or lifestyles that involve extended periods of sitting or standing can increase the risk of varicose veins. When you remain stationary, blood flow in your leg veins may become sluggish, leading to the pooling of blood and increased vein pressure. To mitigate this risk, make a conscious effort to take breaks and move around regularly. If you have a desk job, consider investing in a standing desk or use a footrest to reduce the pressure on your legs while sitting.
Choose the Right Footwear
Your choice of footwear can significantly impact your vein health. Opt for comfortable, low-heeled shoes that provide good arch support. High heels can strain your calf muscles, impeding blood circulation in the legs and contributing to vein issues. Well-fitted shoes with proper arch support encourage healthy posture and can help prevent varicose veins.
Watch Your Diet
Your diet can influence your risk of developing varicose veins. A diet rich in fiber can help prevent constipation, a condition that can exacerbate vein problems. High-fiber foods like fruits, vegetables, and whole grains promote regular bowel movements and healthy digestion. Additionally, maintaining a diet low in sodium can reduce water retention, which can contribute to swelling and added pressure on the veins.
Stay Hydrated
Adequate hydration is essential for maintaining proper blood volume and preventing blood from pooling in your veins. Drinking plenty of water ensures that your blood remains fluid and flows smoothly, reducing the risk of venous issues. Drink at least eight glasses of water a day, and consider consuming hydrating foods like fruits and vegetables to support your fluid balance.
Avoid Crossing Your Legs
Crossing your legs while sitting may be a common habit, but it can restrict blood flow and increase pressure on your veins, particularly in the thigh and calf areas. This restriction can hinder healthy circulation and contribute to varicose veins. Instead of crossing your legs, sit with your feet flat on the floor and occasionally alternate crossing your ankles if needed. This helps maintain unrestricted blood flow in your legs and reduces the risk of vein-related problems.
Ensure Your Vein Doctor Diagnoses & Treats Chronic Venous Insufficiency During the Primary Treatment
Chronic Venous Insufficiency (CVI) is often the root cause of most vein problems, including varicose veins and spider veins. It occurs when the valves in your leg veins fail to function correctly, causing blood to flow backward and pool in the veins. This condition can lead to increased pressure in the veins, weakening the vessel walls and causing them to bulge and become visible as varicose veins. While varicose veins themselves can be treated, it’s essential to understand that unless the underlying CVI is addressed, the risk of recurrence remains high.
CVI is an underdiagnosed condition, primarily because its early signs and symptoms, such as leg pain, swelling, and heaviness, are often misattributed to other factors like aging or overexertion. This misdiagnosis can lead to vein doctors solely focusing on treating the visible varicose veins without addressing the underlying issue, resulting in a high rate of recurrence.
At Long Island Vein Treatment, our approach goes beyond surface-level vein care. We prioritize the accurate diagnosis and treatment of CVI during the primary treatment phase. By utilizing advanced diagnostic techniques like duplex ultrasound, we identify the precise areas of venous insufficiency. This allows us to develop personalized treatment plans that not only target visible varicose veins but also address the root cause – CVI. Our board-certified vein doctors employ minimally invasive procedures like endovenous laser ablation or radiofrequency ablation to treat CVI effectively, ensuring that you have the best chance of long-term vein health.
Contact Long Island Vein Treatment for Personalized Varicose Vein Treatments
Varicose veins can be both uncomfortable and unsightly, but with the right strategies and medical interventions, you can effectively prevent them from coming back. Long Island Vein Treatment is committed to providing you with top-notch vein care, backed by our team of board-certified vein doctors and a range of minimally invasive treatment options. By following the prevention strategies outlined in this article and seeking our expertise when needed, you can maintain vascular health. Don’t hesitate to reach out to us for a consultation — we offer free insurance verification even before your first appointment!