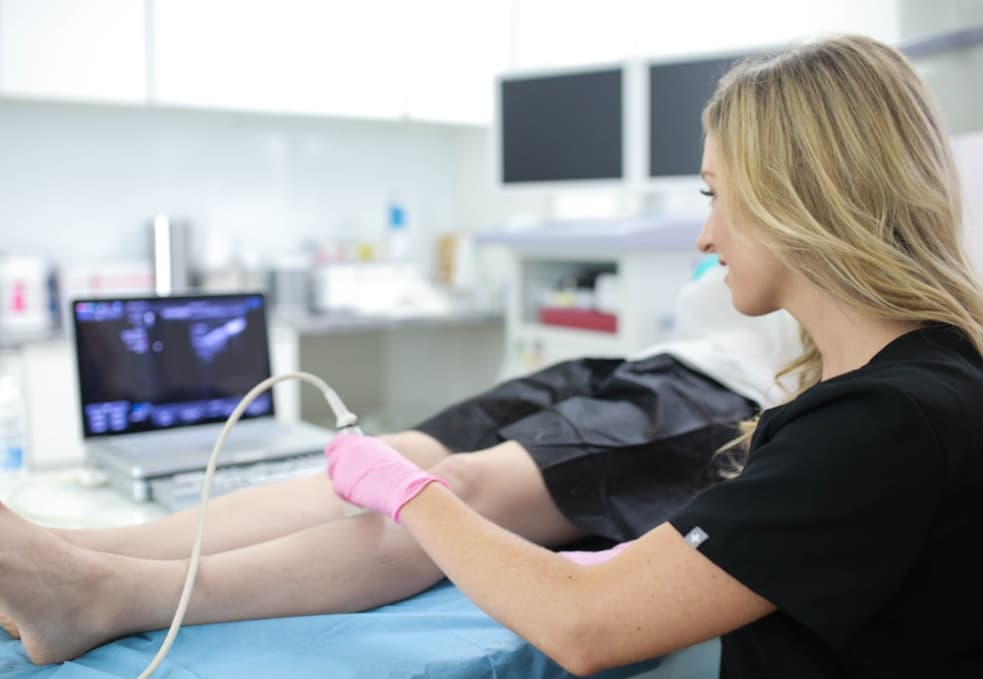
If you’ve been dealing with varicose veins, you may be surprised to learn that these unsightly and often painful veins are more than just a cosmetic concern. Varicose veins can be a sign of underlying vascular issues that can have a significant impact on your overall health. At Long Island Vein Treatment, our team of board-certified vein doctors is here to help you understand the link between varicose veins and other health conditions and provide you with the best minimally invasive vein treatments available.
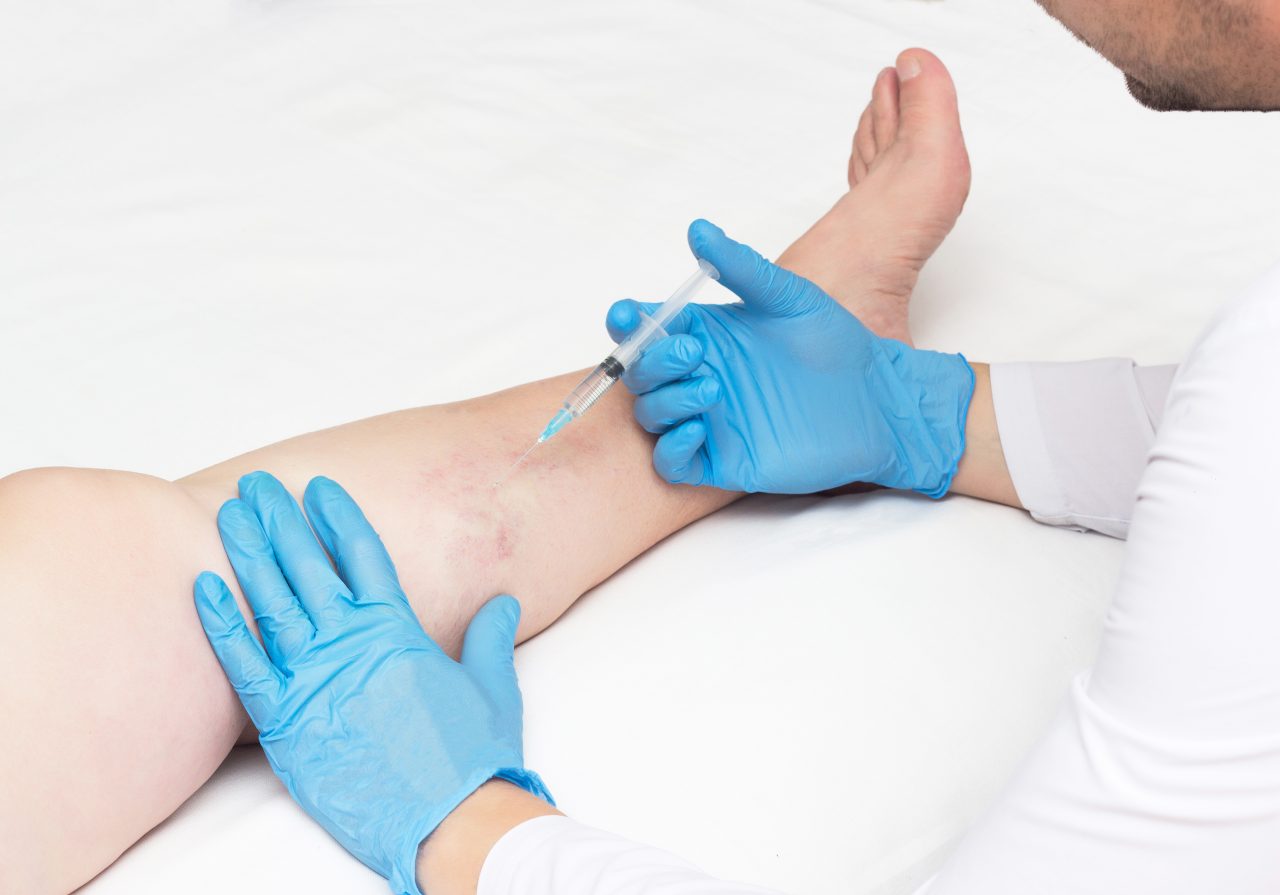
What Are Varicose Veins?
To comprehend the link between varicose veins and other health conditions, it’s essential to understand what varicose veins are and how they develop. Varicose veins are swollen, twisted veins that typically occur in the legs. They usually look like dense, knotted, twisted ropes bulging out of the skin’s surface. Some people confuse varicose veins with spider veins. While both are vascular issues, spider veins are small, thread-like veins that remain under the skin’s surface, whereas varicose veins always bulge out of the skin’s surface.
Varicose veins are a result of damaged valves within the veins. Healthy veins have valves that prevent the backward flow of blood, ensuring that it flows towards the heart. When these valves become weak or damaged, blood can flow backward due to gravity and pool in the veins, causing them to enlarge. The continued accumulation of blood in leg veins eventually leads to varicose veins and spider veins.
Varicose Veins & Chronic Venous Insufficiency (CVI)
In a healthy circulatory system, blood flows smoothly through the veins, carrying oxygen and nutrients to various parts of the body and returning deoxygenated blood to the heart and lungs for reoxygenation. This process is facilitated by a network of valves within the veins that ensure blood flows in one direction—toward the heart. These valves open to allow blood to move upward and then close to prevent it from flowing backward. This efficient system maintains optimal circulation and minimizes the risk of blood pooling in the lower extremities.
Venous insufficiency occurs when the valves in the veins become weakened or damaged, causing a disruption in the normal flow of blood. In this condition, blood can flow backward and accumulate in the veins of the legs. This leads to increased pressure within the veins, causing them to become dilated, twisted, and bulging—manifesting as varicose veins. Essentially, venous insufficiency impedes the proper return of blood to the heart, resulting in a range of vascular problems. Consequently, varicose veins are often an outward sign of an underlying vein disease like chronic venous insufficiency.
Signs & Symptoms of Venous Insufficiency:
- Swollen and painful legs
- Heavy and aching sensations in the legs
- Fatigue and restlessness in the legs
- Skin changes, such as darkening or inflammation
- Itching and dryness of the skin
- Ulcers, particularly near the ankles
- Varicose veins and spider veins
- Muscle cramps in the calves
- Throbbing or burning sensations in the legs
Potential Complications of Untreated CVI:
- Deep vein thrombosis (DVT)
- Pulmonary embolism
- Venous ulcers
- Skin infections
- Bleeding from varicose veins
- Lipodermatosclerosis (thickening and hardening of the skin)
- Cellulitis (skin infection)
- Chronic leg pain
- Skin discoloration and scarring
- Reduced quality of life and mobility
Varicose Veins & Restless Leg Syndrome (RLS)
Restless Leg Syndrome, commonly referred to as RLS, is a neurological disorder characterized by an uncontrollable urge to move the legs, often accompanied by uncomfortable sensations such as tingling, crawling, or aching. These symptoms tend to worsen during periods of rest or inactivity and are often most bothersome at night, making it challenging for individuals with RLS to get a good night’s sleep.
Untreated varicose veins and chronic venous insufficiency (CVI) can contribute to the development of RLS. The impaired blood flow and pooling of blood in the lower extremities associated with varicose veins can lead to increased pressure in the leg veins. This elevated pressure can irritate the nerves in the legs, triggering the sensations characteristic of RLS. Additionally, the disruption of normal circulation caused by CVI may contribute to the symptoms and disturbances caused by RLS.
Signs & Symptoms of Restless Leg Syndrome:
- Uncontrollable urge to move the legs
- Unpleasant sensations in the legs, often described as tingling, crawling, or aching
- Symptoms worsen during periods of rest or inactivity
- Symptoms are often more pronounced at night
- Difficulty falling asleep or staying asleep due to leg discomfort
- Relief from symptoms when the legs are moved or stretched
- Fatigue and daytime sleepiness due to disrupted sleep patterns
Lifestyle Tips to Manage RLS:
- Engage in moderate physical activity
- Perform gentle leg stretches to alleviate discomfort
- Establish a consistent sleep routine
- Reduce or eliminate caffeine and alcohol
- Refrain from smoking
- Soak in a warm bath or get a leg massage
- Apply heat or cold packs to your legs
- Employ relaxation techniques like deep breathing and meditation
Varicose Veins & Stasis Dermatitis
Stasis dermatitis occurs due to impaired circulation in the legs, particularly when the valves in the leg veins fail to function correctly. When these valves are compromised, blood can pool in the lower extremities, leading to increased pressure in the veins. This elevation in pressure forces fluid to leak from the veins into the surrounding tissues, resulting in inflammation and damage to the skin. Over time, this chronic inflammation can result in changes to the skin’s texture, including thickening, discoloration, and the formation of open sores or ulcers.
Signs & Symptoms of Stasis Dermatitis:
- Redness and inflammation of the skin, particularly around the ankles and lower legs
- Swelling in the affected areas
- Itching and dryness of the skin
- Skin that feels warm to the touch
- Thickened or leathery texture of the skin
- Formation of open sores or ulcers, especially near the ankles
- Skin discoloration, often appearing brownish or reddish
- Pain or discomfort in the affected areas
- Weeping or oozing of fluid from the skin
- Skin changes that worsen with prolonged standing or sitting
Potential Complications of Untreated Stasis Dermatitis:
- Cellulitis (skin infection)
- Recurrent skin infections
- Development of venous ulcers
- Chronic leg pain and discomfort
- Formation of skin nodules and lumps
- Scarring and skin discoloration
- Reduced quality of life due to persistent skin issues
- Secondary skin conditions such as eczema or psoriasis
- Delayed wound healing and tissue damage
Varicose Veins & Venous Ulcers
Venous ulcers, or venous stasis ulcers, are chronic open sores that typically develop on the lower legs. These ulcers are a painful consequence of CVI and untreated varicose veins. The process begins when CVI leads to high pressure and poor circulation in the leg veins. This results in the pooling of blood and fluid in the lower extremities. When the tissue is deprived of oxygen and nutrients due to poor circulation, it becomes fragile and more susceptible to injury. Furthermore, without proper blood flow, existing wounds can’t heal properly.
Signs & Symptoms of Venous Ulcers:
- Open sores or wounds on the lower legs, particularly near the ankles
- Irregularly shaped ulcerations with uneven edges
- Surrounding skin may appear discolored, often reddish or brown
- Pain or discomfort at the site of the ulcer
- Swelling in the affected leg
- Skin may feel warm to the touch
- Weeping or oozing of fluid from the ulcer
- Foul odor from the wound due to infection or dead tissue
- Slow healing or non-healing wounds
- Development of hardened or scarred tissue around the ulcer
Potential Complications of Untreated Leg Ulcers:
- Infection of the ulcer, leading to cellulitis or abscess formation
- Cellulitis (skin infection), which can spread to other areas of the body
- Osteomyelitis (bone infection) if the infection extends to the underlying bone
- Gangrene (tissue death) in severe cases
- Delayed wound healing and prolonged pain
- Development of additional ulcers in the same or nearby areas
- Reduced mobility and difficulty walking
- Impaired quality of life due to chronic pain and discomfort
- Increased risk of systemic infections if bacteria from the ulcer enter the bloodstream
- Risk of complications such as sepsis, which can be life-threatening
Varicose Veins & Deep Vein Thrombosis (DVT)
Deep Vein Thrombosis, commonly known as DVT, is a potentially life-threatening condition that occurs when a blood clot forms in the deep veins of the body, typically in the legs. These clots can obstruct blood flow and pose a severe risk if they break loose and travel to the lungs, causing a pulmonary embolism. DVT often develops due to various factors, including prolonged immobility, injury, or surgery, but it can also be linked to underlying vein issues.
Untreated varicose veins and chronic venous insufficiency (CVI) significantly heighten the risk of DVT. Varicose veins, characterized by weakened or damaged valves that impede blood flow, lead to pooling of blood in the legs. This stagnant blood can facilitate the formation of blood clots, especially when combined with the inflammation and vascular damage. Over time, these blood clots can dislodge and travel through the bloodstream, potentially causing a pulmonary embolism or other serious complications.
Signs & Symptoms of Deep Vein Thrombosis:
- Swelling in the affected leg, often accompanied by warmth and redness
- Pain or tenderness, typically in the calf but sometimes in the thigh
- Leg cramps or aching, especially when walking or standing
- Skin discoloration, often turning bluish or reddish
- Enlarged and prominent surface veins
- Increased pain when flexing the foot upward (Homans’ sign)
- Unexplained shortness of breath or chest pain
Potential Complications of Untreated DVT:
- Pulmonary embolism (a life-threatening condition where a clot travels to the lungs)
- Post-thrombotic syndrome (chronic leg pain, swelling, and skin changes)
- Vein damage and scarring
- Clot extension into deeper veins
- Increased risk of developing more blood clots in the future
- Reduced blood circulation in the affected leg
- Limb ischemia (reduced blood flow leading to tissue damage)
- Death in severe cases of untreated pulmonary embolism
Treat Varicose Veins at the Earliest Stage Possible
Varicose veins are not merely a cosmetic concern; they can be indicative of underlying health issues that should not be ignored. If you are experiencing varicose veins, it’s essential to seek evaluation and treatment from board-certified vein doctors who understand the potential link between varicose veins and other health conditions.
At Long Island Vein Treatment, we are dedicated to providing you with the highest level of care and expertise. Our minimally invasive vein treatments, thorough diagnostic approach, and convenient locations make it easy for you to take the first step towards healthier legs. You can find our offices at West Islip, Jericho, Port Jefferson, or Hampton Bays, so there’s a medical center for vein treatment near your location, wherever you are. Contact us today to schedule your consultation and request free insurance verification.